1. Introduction: Your Nails as a Window to Your Health
While often viewed through a cosmetic lens, your nails serve as a vital diagnostic indicator of your overall well-being. Changes in the color, texture, or shape of your nails are rarely isolated events; they frequently reflect environmental stressors, personal habits, or underlying systemic health conditions. I understand that these changes can often be a source of significant anxiety or embarrassment, but they are also valuable signals from your body. Maintaining nail integrity requires a proactive partnership between the patient and the clinician, where careful observation leads to early intervention.


Podcast:
Learn More About Nails
Understanding nail health begins with basic anatomy. The nail plate (the hard surface) is produced by the matrix. Specifically, the proximal matrix, located between the cuticle and the first finger joint, forms the top surface of the nail. Because of this, any disease or injury affecting this area leads to visible nail dystrophy or malformation. The lunula is the whitish, crescent-shaped area at the base of the nail; it is part of the distal matrix, which is responsible for the undersurface of the nail. This area is clinically significant, as 75% of nail melanomas arise from the distal matrix and present as pigmented bands. The nail bed—the skin beneath the plate—contributes the remaining third of the nail’s structure. By understanding these components, we can better identify the diverse causes of common nail concerns.
2. Why Are My Nails Changing? Understanding the Causes
Identifying the “root cause” of a nail abnormality is a strategic necessity. Treating only the surface symptoms often leads to recurring issues if the underlying driver—whether it be a lifestyle habit, an infection, or a systemic disease—is not addressed.
Environmental & Lifestyle Factors
Nails are surprisingly porous; they absorb significantly more water than the surrounding skin. This makes them highly susceptible to dryness, which manifests as peeling, thinning, or breaking. When the surrounding skin is dry and scaly, the nail plate follows suit. Furthermore, repeated mechanical trauma—even minor microtraumas from daily tasks—can disrupt the matrix and alter the nail’s growth pattern.
Infections
Biological invaders are common drivers of nail distress.
- Bacteria: Pseudomonas is a frequent culprit, often thriving in damp spaces created when the nail separates from the bed. This is frequently related to “wet work” and repeated exposure to soap and water, which causes maceration—the softening and breaking down of the tissue—of the hyponychium.
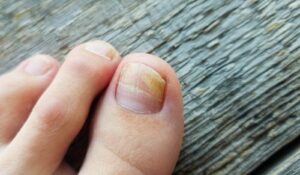
- Fungi & Yeast: Tinea Unguium (fungal) and Candida (yeast) can cause the nail to become thickened, discolored, and crumbly. These infections often gain a foothold following a minor injury to the nail unit.
Internal Health & Genetics
In many cases, the nail acts as a reporter for the rest of the body. Systemic diseases such as thyroid disorders, iron deficiency, psoriasis, and lichen planus can fundamentally change nail production. If internal conditions are suspected, a clinician may order a nutritional panel to check markers such as Zinc, Vitamin D, B3, B12, Folic Acid, and Ferritin. Additionally, some nail traits, such as certain white lines or pigmented bands in darker skin tones, may be linked to genetic factors rather than external damage.
Common Nail Symptoms and Potential Clinical Causes
| Symptom | Potential Clinical Cause |
| Green-black discoloration | Pseudomonas (bacterial) infection |
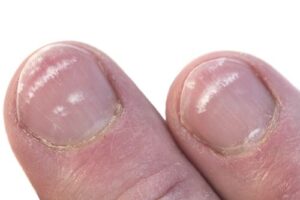
| Horizontal grooves (Beau’s Lines) | Systemic illness or significant body stress |
| Pitting (Ice pick-like depressions) | Psoriasis |
| Painless separation from the bed | Onycholysis (due to moisture, trauma, or medications) |
| White spots or lines | Leukonychia (minor trauma to the matrix) |
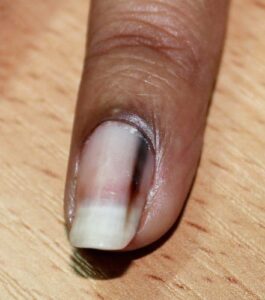
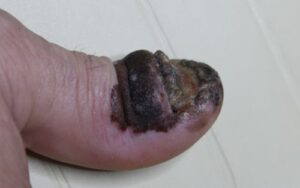
| Purple-black discoloration | Hematoma (collection of blood from trauma) |
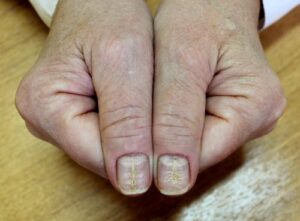
| “Fir tree” pattern/central groove | Median canal dystrophy (habit tic/rubbing) |
Your daily environment acts as a catalyst for these issues. Constant exposure to irritants, chemicals, or moisture can turn a minor genetic predisposition or a small injury into a chronic clinical condition.
3. Who Is At Risk? Identifying Vulnerability Factors
Certain individuals are more prone to nail disorders due to the repetitive nature of their occupations or personal habits. Recognizing these vulnerabilities is the first step toward prevention.
- Service & Healthcare Workers: Gardeners, hairdressers, and healthcare professionals are at high risk for chronic paronychia (nail fold inflammation) and bacterial infections due to repeated exposure to moisture and chemicals.
- Athletes: Runners frequently experience “subungual hematomas”—purple-black bruising under the nail—caused by repetitive pressure and friction within footwear.
- Individuals with Habit Tics: Self-induced trauma, such as compulsive nail-biting or the repetitive rubbing of the nail fold, can lead to permanent changes. For example, “median canal dystrophy” results in a split or “fir tree” appearance due to constant physical manipulation of the growth area.
These behaviors don’t just affect appearance; they compromise the nail’s protective barrier, making it easier for infections to take hold and causing long-term growth disruptions.
4. Recognizing Common Nail Concerns
While many nail changes are benign signs of aging or minor knocks, others are signals that the nail unit is under distress and requires specific interventions.
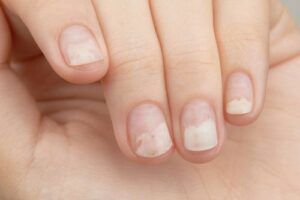
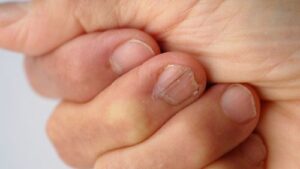
“What Are These White Spots or Lines?”
Known as Leukonychia, these marks are usually the result of minor, often unnoticed trauma to the nail matrix (like aggressive cuticle pushing or nail-biting).
- The “So What?”: These spots are harmless and will eventually grow out. They do not move when the nail is pressed, unlike superficial debris.
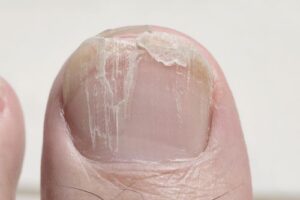
“Why Are My Nails Brittle or Peeling?”
This is often categorized into Onychoschizia (horizontal splitting at the tip) or Onychorrhexis (longitudinal/vertical ridging).
- The “So What?”: Horizontal peeling is often caused by excessive moisture or chemical irritants, while vertical ridges are commonly a sign of aging but can also signal nutritional deficiencies or underlying conditions like lichen planus.
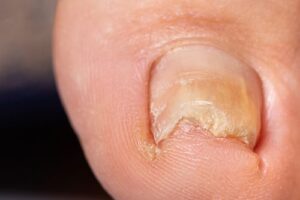
“What Is This Rough, Sandpaper Texture?”
Trachyonychia, or Twenty Nail Dystrophy, is characterized by nails that appear rough, thin, and brittle.
- The “So What?”: Affected nails often have a chalky, matte appearance and lack a normal shine. While it may involve all twenty nails, it is a manifestation of various autoimmune disorders and requires clinical monitoring.
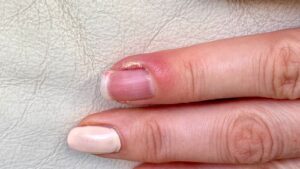
“What Causes Painful Swelling Around the Nail?”
Paronychia presents as redness, swelling, and pain in the nail folds.
- The “So What?”: This is a sign that the skin barrier has been breached. If left untreated, pus can accumulate, potentially leading to an abscess.
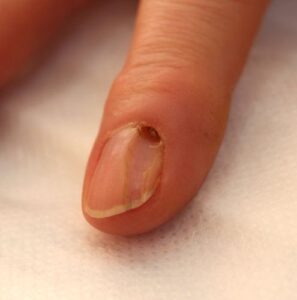
“Why Is My Nail Separating from the Bed?”
Onycholysis is the painless lifting of the nail plate. Common triggers include trauma, moisture, or drug photosensitivity (specifically to tetracyclines).
- The “So What?”: When a nail lifts, it creates a “damp, macerated space” between the nail and the bed. This environment is fertile ground for Pseudomonas bacteria, which causes the nail to turn green-black.
5. How Can I Care for My Nails? Non-Prescription & Home Solutions
Restoring nail health begins with consistent, daily self-care. The following protocols are designed to rebuild the nail’s natural defenses.
- Moisturization Protocol: Use ointment-based emollients (thick, heavy products like petroleum jelly) rather than thin lotions. For maximum effectiveness, apply the ointment immediately after hand washing while the nails and cuticles are still wet to trap moisture within the nail plate.
- Irritant Avoidance: Minimize hand washing where possible and avoid hand sanitizers containing Triclosan. Avoid nail cosmetics and aggressive manicuring, as these can further dehydrate or traumatize the matrix.
- Home Remedies for Infection:
- For Pseudomonas (Green nails): Create a solution of 1 part bleach to 3 parts sterile water. Apply this under the nail three times a day.
- For Fungal concerns: Applying vinegar or apple cider vinegar under the nail is a recognized home-care strategy to create an environment less hospitable to fungi.
While Biotin is frequently marketed for nail growth, the FDA has issued a warning regarding its use. Biotin can significantly interfere with essential medical lab tests, leading to falsely low results in cardiac evaluations (Troponin) and inaccurate thyroid testing. Always inform your doctor if you are taking Biotin.
6. When to See a Professional: Monitoring for Serious Signs
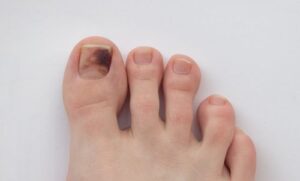
Early detection is the most critical factor in treating serious conditions like nail melanoma. While most pigmented bands (melanonychia) are benign—particularly in darker skin tones—it is vital to distinguish between adult and pediatric cases. In children, pigmented bands can often look irregular as they grow, and clinicians have a higher “threshold to react.” However, in adults, new or changing lines require immediate attention.
Checklist of Concerning Signs:
- Hutchinson’s Sign: Pigment that extends off the nail plate and onto the surrounding skin, such as the cuticle or nail folds.
- The Triangle Sign: A pigmented band where the proximal dimension (at the base near the cuticle) is wider than the distal edge (at the tip of the finger).
- Size & Symmetry: Any band wider than 3mm, or one that shows asymmetry in its borders or color.
- New Changes: Any new pigmented line in an adult, or a band that is changing rapidly in size or color.
In simple terms, if you notice a dark line that is wider at the bottom than the top, or if the color seems to be “bleeding” into the skin around your nail, seek a professional evaluation immediately. While most nail issues are manageable with home care, these high-risk signs require expert clinical diagnosis to ensure the best possible outcome.
