If you have noticed persistent, symmetrical brown patches appearing on your face, please know that your experience is a common one. As a dermatologist, I often see the frustration these changes cause. While melasma is entirely asymptomatic—meaning it does not cause pain, itching, or physical discomfort—its presence can be deeply personal. Understanding that this is a specific medical condition is the first step toward a specialized management approach that goes far beyond standard skincare.






1. What is Melasma?
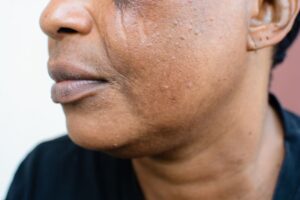
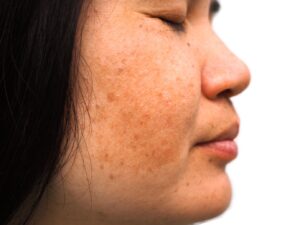
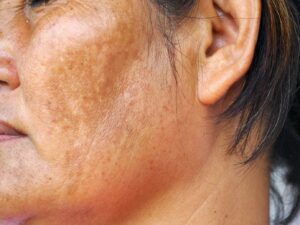
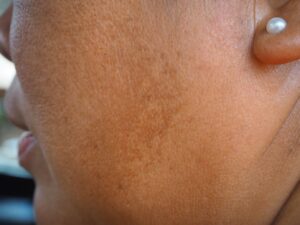
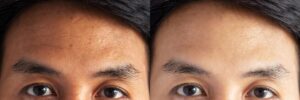
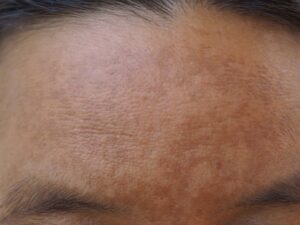
Melasma is a form of hyperpigmentation that typically appears as symmetrical brown patches on the face and neck. Unlike other skin spots that may appear randomly, melasma is characterized by its balanced, “mirror-image” distribution. One of the hallmarks I look for during a clinical exam is the sparing of the nasolabial folds (the lines running from the nose to the corners of the mouth); this unique feature helps us distinguish melasma from other inflammatory conditions.
Clinically, the intensity of the pigment can range from very faint to quite dark, often following three distinct patterns:
- Centrofacial: The most common pattern, appearing on the forehead, nose, cheeks, upper lip, and chin.
- Malar: Focusing primarily on the cheeks.
- Mandibular: Appearing along the jawline.
The “So What?” Layer: Recognizing these patterns is essential because it allows us to target treatment effectively. By identifying whether your melasma is concentrated on your upper lip or spreading across your forehead, we can better monitor the condition’s progression and tailor protection strategies to the areas most affected by environmental triggers.
2. Uncovering the Causes (Etiology)
In dermatology, we use the word “etiology” to describe the underlying cause of a condition. For melasma, the cause is “multifactorial,” meaning several triggers work together to stimulate your skin’s pigment-producing cells. Understanding these triggers is the first step in regaining control over your skin health.
The primary factors contributing to melasma include:
- Genetic Predisposition: Your DNA plays a major role in how your skin reacts to the environment.
- Light Exposure: This includes UV radiation from both the sun and artificial sources, as well as visible light.
- Hormonal Influences: Pregnancy (specifically during the 2nd or 3rd trimester), oral contraceptives, and estrogen-progesterone therapies are major drivers.
- Secondary Factors: Thyroid dysfunction and certain “phototoxic” medications—such as the blood pressure medication Diltiazem or the diuretic HCTZ—can also trigger pigmentation.
The “So What?” Layer: We often speak of a “hormonal bridge” in melasma management. While patches may appear during pregnancy and fade after delivery, they can also persist long after you have stopped taking oral contraceptives. This happens because the initial hormonal surge “primes” the skin, making it more sensitive to other triggers like sunlight for years to come. Identifying these triggers helps us ensure we aren’t mistaking melasma for “Post-inflammatory hyperpigmentation” (pigment left after a rash) or a simple reaction to a new medication.
3. Risk Factors and the Power of Prevention
While anyone can develop melasma, certain biological and environmental factors significantly increase your susceptibility. My role is to help you understand your unique risk profile so we can build a proactive defense.
According to clinical data, high-risk groups include:
- Skin Type and Origin: Melasma is most prevalent in individuals of Hispanic, Latin American, Middle Eastern, Asian, and African origin. We specifically look at Fitzpatrick Skin Phototypes II–V. In plain English, this refers to skin that ranges from fair-beige to dark brown—skin that typically tans easily or has a naturally olive to deep brown tone. These skin types have more active pigment-producing cells.
- Gender: Women are affected significantly more often than men, largely due to the hormonal influences mentioned above.
- Environment: High levels of cumulative sun exposure are a primary driver for all risk groups.
The “So What?” Layer: It is important to realize that “prevention” is not about changing your genetics. Instead, it is about managing the environmental triggers you can control. Sun exposure is the most significant and controllable risk factor we have. By understanding your biological risk, you can adopt a more proactive stance toward protection before the pigmentation deepens or spreads.
4. Taking Control: At-Home Care and Non-Prescription Treatments
Professional treatments like chemical peels or prescription creams are only as effective as the foundation of care you build at home. Think of at-home care as the daily maintenance that allows medical interventions to succeed.
Paramount Sun Protection
Sun protection is the most critical element of management. Because even a small amount of light can trigger a relapse, I recommend a “multimodal” approach:
- Physical Barriers: Wide-brimmed hats and sunglasses provide essential shade for the face and the delicate skin around the eyes.
- Pigmented Sunscreens: You must use a zinc oxide sunscreen that specifically includes iron oxide.
The “So What?” Layer: Most standard sunscreens only block UV rays. However, melasma is also triggered by visible light. Iron oxide acts as a physical barrier that blocks this visible light, providing a level of protection that standard “clear” sunscreens simply cannot offer.
Non-Prescription/OTC Topical Agents
Beyond protection, several over-the-counter (OTC) ingredients can help manage pigment:
- Antioxidants: Vitamins C and E help neutralize environmental damage.
- Pigment-Correcting Agents: Ingredients like Rucinol and Cysteamine compounds work differently than traditional harsh bleaches; they help regulate the pigment production process more gently.
- Exfoliants: Amino acid fruit peels designed for home use can help shed surface-level pigment.
5. The Journey Ahead: Maintenance and Outlook
Melasma is a chronic condition, and it is important to set realistic expectations. There is no “instant fix,” and the condition is notorious for relapsing if maintenance is paused.
During a clinical visit, we may use a Wood’s Light Exam to classify your melasma into types:
- Epidermal (Surface): Pigment is in the top layer of skin. This type usually responds more quickly to treatment.
- Dermal (Deep): Pigment is deeper in the skin. This type is often resistant to standard bleaching agents and takes longer to treat.
- Mixed: A combination of both surface and deep pigment.
The “So What?” Layer: While the word “chronic” can sound daunting, it actually serves as a roadmap. “Success” in melasma management isn’t just about the initial clearing of the skin; it is about the persistence of your routine. By combining rigorous sun protection, effective home care, and professional guidance, we can successfully manage the condition over the long term. If home care is not reaching your goals, we can then discuss advanced options like triple-combination prescription creams or in-office procedures.
6. Key Terms to Know (Glossary)
Medical terminology can be confusing. This glossary is designed to empower you during your clinical visits.
- Hyperpigmentation: An increase in melanin (pigment) in the skin, resulting in patches darker than the surrounding area.
- Symmetric: Occurring in a mirror-like pattern on both sides of the face.
- UV Radiation: Ultraviolet radiation from sunlight or artificial sources; a primary trigger for pigment.
- Wood’s Light Exam: A diagnostic test using a specific light that helps determine the depth of the pigment (epidermal vs. dermal).
- Relapse: The recurrence of dark patches after they have improved or cleared.
- Phototoxic: A property of certain medications that makes your skin more sensitive to light damage.
- Multimodal: A treatment approach that uses several different methods at once (e.g., hats + sunscreen + creams) to achieve the best result.
