Understanding Bullous Impetigo
Discovering unexpected blisters on yourself or your child can be a source of significant concern. It is important to remember that bullous impetigo, while highly contagious, is a common and manageable bacterial skin infection. As a healthcare specialist, my goal is to provide you with the knowledge to recognize the symptoms early and take the necessary steps toward a full recovery.
Podcast:
Learn More About Bullous Impetigo
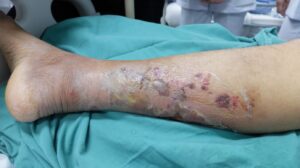
Bullous impetigo occurs in the most superficial part of the skin, specifically the epidermal granular layer. It is characterized by dome-shaped, thin-walled blisters (known as bullae) that often appear translucent and flaccid. These blisters typically contain a yellow or pus-like fluid and are prone to rupturing spontaneously, leaving behind shiny red skin or superficial erosions. While these blisters can appear anywhere on the body, they are most frequently found on the face, arms and legs (extremities), trunk, and buttocks. Although the appearance can be startling, the prognosis is excellent; with professional care and diligent hygiene, the condition typically resolves without long-term complications.
The Biological Cause
Effectively treating an infection requires understanding the microscopic “engine” driving it. The primary culprit behind bullous impetigo is the bacterium Staphylococcus aureus. Understanding how this specific bacterium behaves is the first step in stopping its spread.
Staphylococcus aureus produces specialized substances known as exfoliative toxins. You can think of these toxins as “chemical scissors” that specifically target and disrupt the bonds holding skin cells together in the granular layer. This process, known as pathogenesis, is why bullous impetigo looks different from other skin conditions. While other infections might cause simple crusting, these toxins create a physical gap between skin layers where fluid collects, resulting in the characteristic thin-walled blisters. Because these blisters are so fragile, they often break easily, which is why identifying the underlying cause is vital for choosing the right treatment.
Who Is At Risk and How It Spreads
From a public health standpoint, identifying risk factors is the most effective way to protect vulnerable groups—particularly young children, who are the most frequently affected. By recognizing how the bacteria travel, we can create a “safety barrier” around our families. The infection primarily spreads through the following methods:
- Direct Contact: Transmission most often occurs through physical touch with an infected person or direct contact with the fluid from a ruptured blister.
- Personal Grooming Habits: For adolescents and adults, a major risk factor is the repeated use of the same razor blade to shave the arms or legs, which can spread the bacteria across the skin surface.
- Close-Contact Environments: Schools and nurseries are common sites for outbreaks due to the high frequency of interaction between children.
Understanding these real-world risks allows us to move from concern to action, implementing specific self-care and hygiene measures to break the cycle of infection.
Managing the Infection: Your Front-Line Defense
While your doctor will provide the necessary medical treatment, your home-based hygiene practices are the “front line” in stopping community spread and preventing reinfection. To manage the infection effectively, please adhere to these scannable guidelines:
- Strict Hand Hygiene: Wash your hands thoroughly with soap and water both before and after applying any prescribed antibiotic creams or touching the affected skin.
- Dedicated Skin Care: Avoid picking at or touching the blisters. When washing the area, use a fresh, clean cloth every single time, and do not use that cloth on any other part of the body.
- Household Sanitation:
- Do not share personal items such as towels, razors, or clothing.
- Launder daily all clothing, towels, and bedding used by the infected person in hot water to ensure the bacteria are destroyed.
- Mandatory Isolation: To protect the community, children must stay home from school or nursery until they have completed at least 24 hours of their prescribed antibiotic treatment.
Professional Diagnosis and Next Steps
While the guide above helps you manage the condition, a professional clinical diagnosis is non-negotiable. Bullous impetigo can often look like other conditions, such as Herpes Simplex, Shingles, or Childhood Bullous Pemphigoid (which presents with “tense” blisters rather than the thin-walled, flaccid ones seen here). A healthcare provider will examine the blisters and may take a skin swab for testing to ensure the correct treatment is chosen.
Clinical Expectations:
- Testing: In cases where the infection keeps returning, your doctor may perform a nasal swab. This is to check for nasal carriage, a situation where Staphylococcus aureus lives in the nasal passages without causing symptoms, acting as a hidden reservoir for future skin outbreaks.
- Medication: Recovery relies on completing the full course of prescribed antibiotics. Common treatments include Cephalexin or Amoxicillin. If your doctor suspects MRSA (a resistant strain of bacteria) or if you have a penicillin allergy, they may prescribe Bactrim or Doxycycline.
By combining professional medical diagnosis with the diligent hygiene measures outlined in this guide, you can ensure a swift recovery and maintain a healthy environment for your household.
