Quick Summary: Lichen simplex chronicus, also known as neurodermatitis, is a chronic skin condition driven by a self-perpetuating itch-scratch cycle that leads to thickened, leathery skin patches [cite: 1965, 2038]. The most effective solution is to break the habit of scratching through physical barriers and targeted medical treatments to allow the skin to heal [cite: 2003, 2041].
What Is Causing This Thickened Patch on My Skin?
Understanding the link between your nerves and your skin is a strategic first step in managing neurodermatitis [cite: 2041]. This condition stems from a chronic itch-scratch cycle [cite: 1972]. You can think of it as a “misguided guard” response—an initial itch from something like a bug bite, sweat, or stress triggers scratching [cite: 1972, 1973]. This scratching activates the brain’s reward center, which reinforces the habit and makes it difficult to break, even as the skin thickens for protection [cite: 1974].
Identifying the primary trigger is the “So What?” factor in your recovery. Because the skin becomes leathery (lichenified) and the nerves more sensitive, the patch becomes even itchier the more it is rubbed, creating a persistent loop of irritation [cite: 1967, 1974].




Podcast:
Learn More About Neurodermatitis
Understanding the Condition: Primary vs. Secondary
Distinguishing how the itch started is essential for long-term control. Neurodermatitis can either develop on previously healthy skin or be triggered by an existing condition [cite: 1972].
| Type | Key Characteristics |
|---|---|
| Primary LSC | Develops on what was initially normal skin, often triggered by stress or minor irritants [cite: 1972, 1973]. |
| Secondary LSC | Triggered by underlying conditions like atopic dermatitis, psoriasis, or dry skin (xerosis) [cite: 1972]. |
Am I at risk for neurodermatitis?
If you are struggling with a persistent, thickened patch, it is important to remember that this condition is a neurological and inflammatory response, not a reflection of hygiene [cite: 1974, 2045]. Susceptibility is often a mix of your medical history and lifestyle factors [cite: 1976].
- Existing Skin Conditions: Individuals with atopic eczema or psoriasis are at higher risk [cite: 1978, 1981].
- Psychological Factors: High stress levels and anxiety disorders are powerful drivers of the itch-scratch cycle [cite: 1977, 1982].
- Environmental Triggers: Heat, sweat, or wearing tight clothing made of wool or synthetic fabrics can initiate the itch [cite: 1973, 1983].
- Nerve Sensitivity: Previous nerve injuries can make specific areas of the skin more prone to chronic itching [cite: 1985].
Where and How It Appears on My Body
The “location” of a patch is a strategic clue, as neurodermatitis almost always appears in areas that are easily reachable for scratching [cite: 1968].
- Common Hotspots: The back of the neck, scalp, wrists, and ankles [cite: 1969].
- The “Heel Habit”: It is common for individuals to use their opposite heel to scratch an itchy patch on the shin or ankle [cite: 1969, 2084].
- Sensitive Areas: It can also affect the eyelids, or the genital and perianal regions [cite: 1969, 1970].
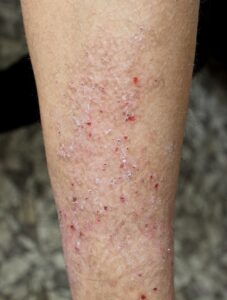
- Clinical Clues: Look for “lichenification”—thickened skin with exaggerated markings—and visible scratches (excoriations) [cite: 1965, 1966, 2046].
Solutions I Can Try at Home
Consistent daily self-care is the foundation of breaking the physical habit of scratching and allowing the skin barrier to repair [cite: 2003, 2041].
- Create Physical Barriers: Use bandages or dressings over the affected area to prevent your fingers from reaching the skin [cite: 2005, 2022].
- Keep Nails Trimmed: Short nails minimize the damage you can do if you scratch subconsciously, especially during sleep [cite: 2007].
- Barrier Repair: Apply thick emollients frequently to hydrate the skin and provide a protective shield [cite: 2011].
- Manage Your Environment: Wear loose-fitting clothing and avoid known irritants or high-heat situations that trigger the itch [cite: 2008, 2009].
When Should I See a Dermatology Provider?
A professional diagnosis is the only way to break a severe cycle of neurodermatitis and rule out other conditions that may look similar [cite: 2040].
Seek Professional Help if You Notice These “Red Flags”:
- Severe Disruption: The itching is so intense it is preventing you from sleeping or interfering with your daily life [cite: 2033].
- Secondary Infection: You notice pus, bleeding, or increasing pain in the patch [cite: 2049, 2053].
- Widespread Symptoms: The itching or patches are spreading significantly beyond one localized area [cite: 1994].
- Treatment Failure: Over-the-counter moisturizers are not helping, and the skin remains thickened and leathery [cite: 2036].
Frequently Asked Questions
- Q: Why does scratching feel so good if it’s bad for me?
A: Scratching actually activates the brain’s reward center, which provides temporary pleasure but reinforces the habit, making the cycle harder to break [cite: 1974]. - Q: Will my skin ever look normal again?
A: Yes. Once the scratching stops and the inflammation is treated, the skin can gradually thin and soften, though some color changes (lighter or darker spots) may remain [cite: 1966, 2036]. - Q: Can stress really cause a skin rash?
A: Absolutely. High stress and anxiety can directly trigger the nerves to send itch signals, starting the cycle that leads to neurodermatitis [cite: 1973, 1982].
The long-term outlook for neurodermatitis is manageable through persistence. Success lies in identifying your triggers, committing to not scratching, and maintaining consistent skin barrier support.
