1. Introduction: Navigating Your Diagnosis with Confidence
Receiving a diagnosis of a blistering skin condition can be a deeply unsettling experience. It is natural to feel overwhelmed by the physical changes and the uncertainty of what lies ahead. However, as a patient educator, I want to reassure you that you are not alone, and education is your most effective tool for regaining control. Understanding the “how” and “why” behind your symptoms allows you to partner more effectively with your healthcare team and manage your recovery with confidence. Pemphigoid is not a single disease but a group of autoimmune conditions characterized by the formation of blisters just beneath the top layer of skin. While the appearance of these blisters can be startling, they are the result of a specific immune response that we can address with modern medicine. The first step toward healing is understanding the underlying biological cause of the condition.
Podcast:
Learn More About Pemphigoid
2. What Causes Pemphigoid? Understanding the Science of Your Skin
Understanding the etiology—or cause—of Pemphigoid is a strategic part of your journey. When you understand the biological mechanism at play, the treatments your doctor prescribes (such as those that calm the immune system) make much more sense. The condition is caused by a breakdown in the body’s internal “glue.” In healthy skin, the outer layer (the epidermis) is held tightly to the deeper layer (the dermis) by specialized proteins. In Pemphigoid, the immune system mistakenly produces autoantibodies that target these proteins, specifically BP180 (Type XVII collagen) and BP230 . When these proteins are attacked, the structural connection fails, creating a gap where fluid collects and forms a blister. To better understand this process, it helps to identify the specific components involved:
- Autoantibodies: These are proteins produced by your immune system. Instead of attacking germs, they mistakenly target your body’s own healthy structural proteins.
- Keratinocytes: These are the primary skin cells of your outer layer. In Pemphigoid, these cells lose their “grip” on the deeper layers because the proteins holding them in place are being attacked.
- Dermal-Epidermal Junction (DEJ): This is the precise “meeting point” or interface between the epidermis and the dermis. Because this connection point is relatively deep, the blisters that form are thicker and tougher than those seen in other conditions. This deep-seated separation is why Pemphigoid blisters are “tense” and do not easily break, a key detail that helps your doctor make an accurate diagnosis.
3. Who Is At Risk? Identifying Factors and Prevention
Identifying risk factors is crucial for early detection. When patients and families are aware of the common profiles associated with Pemphigoid, they can seek specialized care sooner, preventing the condition from progressing to a more severe state.
Am I at Risk?
Pemphigoid primarily affects older adults, with the majority of cases occurring in individuals between 60 and 80 years old. While a rare form exists in children—usually with a very favorable outlook—it remains predominantly a condition of later life.Clinical research has identified a significant connection between Pemphigoid and specific neurological health markers. Individuals with a history of the following conditions are at a statistically higher risk:
- Stroke
- Dementia
- Parkinson’s disease
- Epilepsy
- Multiple sclerosis
The “So What?” regarding these risk factors is vital for families: if you are caring for a loved one with cognitive impairments like Dementia , you must be their “eyes and ears.” Because they may not be able to effectively report symptoms like itching, family members should regularly check for skin redness or hives. While Pemphigoid cannot be “prevented” through lifestyle changes, early awareness of these risks allows for a faster diagnosis and immediate treatment, preventing widespread skin involvement.
4. Recognizing the Signs: What Does Pemphigoid Look Like?
Recognizing the symptoms of Pemphigoid early is a strategic advantage. Catching the condition before it progresses to the full blistering stage leads to faster intervention and less physical discomfort.
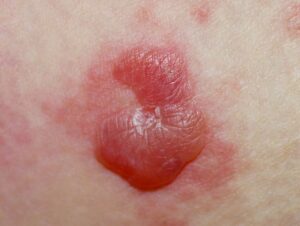
The Early Stage
In its beginning phases, Bullous Pemphigoid (the most common form) often mimics other conditions. It typically starts with localized areas of erythema (redness) and intense pruritus (itching). You may notice swollen, hive-like plaques. Because of this, the condition is frequently misdiagnosed as standard hives in the early weeks.
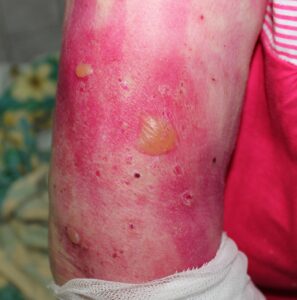
The Blistering Stage
As the condition progresses, “Bullae” (large blisters) begin to appear. These are:
- Tense and Fluid-Filled: Because the target proteins are deep at the Dermal-Epidermal Junction, the blisters are firm and maintain their structure even when compressed.
- Size: They typically range from 1 to 7 centimeters.
- Negative Nikolsky’s Sign: This is a clinical hallmark. Because the “glue” that is failing is deep, the surface skin remains tough; it does not slide off or shear away when gentle pressure is applied near the blister. These signs typically appear on the abdomen, the groin, and the flexor surfaces (the inner folds of the elbows and knees). Important Distinction: In the most common form (Bullous Pemphigoid), the mucous membranes—such as the mouth or eyes—are typically not involved. However, if you notice persistent sores in the mouth or eyes, you may have a variant called Mucous Membrane Pemphigoid, or a drug-induced version of the condition. Always inform your doctor if these areas are affected.
5. Managing Your Condition: Self-Care and Skin Protection
While medical treatments are essential, your daily skin management is the “So What?” layer of care that determines your comfort and healing speed. How you handle your skin daily is just as important as the medications you take.Based on the typical cycle of Pemphigoid, use the following coaching strategies for daily management:
- Protect Intact Blisters: Because these blisters are “tense,” they serve as a natural sterile bandage for the skin underneath. Avoid trauma, and do not squeeze or pop them.
- Anticipate the Healing Cycle: Expect a blister to remain intact for approximately one week before it ruptures. Once it breaks, it leaves behind an “eroded” area. Fortunately, these eroded areas typically heal relatively quickly. Keep them clean and protected according to your doctor’s instructions.
- Maintain a Symptom Log: I recommend keeping a daily diary to track your levels of pruritus (itching) and erythema (redness). Noting whether these sensations are increasing or decreasing is the most effective way to monitor your disease activity and determine if your treatment plan is working.
Understanding Your Treatment Options
Medical care typically begins with Topical Corticosteroids or anti-inflammatory antibiotics like Tetracyclines (Doxycycline or Minocycline), often paired with Nicotinamide. If these are not sufficient, your doctor has a wide range of other options, including:
- Methotrexate (often an initial consideration).
- Dupilumab (a biologic that works rapidly to control itching).
- Systemic Steroids (like Prednisone).
- Rituximab (for cases that do not respond to other treatments).With proper management, the prognosis for many patients is favorable. By combining clinical treatments with diligent self-care, the condition can be successfully brought under control.
6. Glossary of Terms for Your Next Appointment
To help you advocate for your health during your next dermatology visit, here are the most high-value terms to know:
- Autoimmune Disorder: A condition where the immune system mistakenly attacks the body’s own healthy tissues.
- Biopsy: The removal of a small skin sample to be examined under a microscope to confirm a diagnosis.
- Bullae: Large, fluid-filled blisters (0.5 cm or larger) that characterize the condition.
- Dermal-Epidermal Junction (DEJ): The specific layer where the epidermis meets the dermis; this is where Pemphigoid blisters form.
- Erythema: Clinical redness of the skin caused by inflammation.
- Nikolsky’s Sign: A test where pressure is applied to the skin. In Pemphigoid, this is negative , meaning the skin does not easily peel away.
- Pruritic: The medical term for skin that is intensely itchy. Use this guide as a tool for communication with your healthcare provider. By understanding the science and the physical signs of Pemphigoid, you are better equipped to navigate your recovery with confidence.
